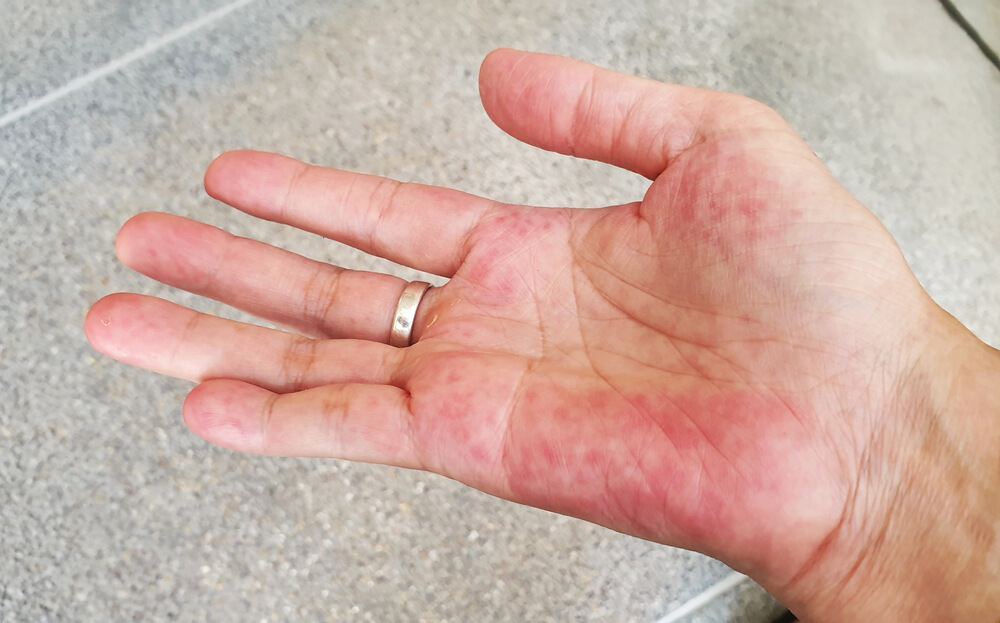
Lupus, or systemic lupus erythematosus (SLE), is an autoimmune disorder where the body produces antibodies against itself. Antibodies are proteins that are usually produced by the body to attack foreign things, such as bacteria and viruses. But in lupus, the antibodies (or autoantibodies) attack the cells of the body. This ‘attack’ causes the variety of symptoms that we see in lupus, including joint pain, rash, lung disease, mouth sores, kidney damage, brain damage, and so on.
The American College of Rheumatology has designated 11 symptoms/signs that are used for the diagnosis of the disease. Most rheumatologists use these criteria for the diagnosis of lupus. A patient has to have at least four of the 11 designated symptoms/signs to be diagnosed with lupus. The symptoms/signs in the diagnostic criteria include:
- Malar rash
- Discoid rash
- Photosensitivity
- Oral ulcers
- Arthritis (in at least two joints)
- Serositis (which is inflammation of the lining of the lungs and/or heart)
- Kidney disease
- Neurologic disease (usually seizures or psychosis)
- Hematologic (blood) disorder, including low white blood cells, low hemoglobin (due to destruction of red blood cells), low platelets, or low lymphocytes (one of the types of white blood cells)
- Abnormal immunologic laboratory results, such as anti-dsDNA, anti-SM, antiphospholipid antibody, lupus anticoagulant, or a false positive test for syphilis
- Abnormal titer of ANA (antinuclear antibody)
In recent years, doctors have been able to diagnose lupus earlier because of the capacity of laboratories to detect these abnormal immune tests with much more accuracy and increased sensitivity.
For more information about lupus, please visit http://www.lupus.org/ or http://www.hopkinslupus.org.
Adahli E. Massey, MD, FACR